
From brain shift to precision: the role of intraoperative MRI in glioma surgery
Value and limits of conventional intraoperative MRI
In 1994, intraoperative MRI (iMRI) was introduced to address this challenge. Studies have shown that iMRI can enhance tumor resection and support safer surgical decision-making. According to the latest research, iMRI increases surgeons' likelihood of achieving gross-total resection (GTR) by 5.4 times compared to conventional navigation1. Patients with GTR had a median progression-free survival of 16.0 months, compared to 9.7 months after subtotal resection.
Despite these better outcomes iMRI remains available only in a limited number of specialized hospitals due to the need for large, dedicated spaces, complex infrastructure, and workflow interruptions caused by transferring the patient for MRI during surgery.
Study Observations from the first 100 cases of intraoperative MRI - experiences, trends and short-term outcomes2 suggests that iMRI led to continuation of the procedure in 50% of cases, primarily because residual pathological tissue was detected but with those conventional MRI systems, high-field machines with superconducting magnets of 1.5 or 3 Tesla, performing an intraoperative check is a logistical challenge as moving a patient from the operating room to the scanner and back can take up to an hour. Given the length and complexity of neurosurgical procedures, surgeons are often limited to a single intraoperative scan.
How technology can eliminate disruptions in the OR
“Most neurosurgeons believe intraoperative MRI is valuable, but many don’t use it because it disrupts surgery, primarily due to the need to transfer the patient for MRI imaging” – said Dr. Roberto Rafael Herrera, Chief of Neurosurgery at Clínica Adventista Belgrano in Buenos Aires.
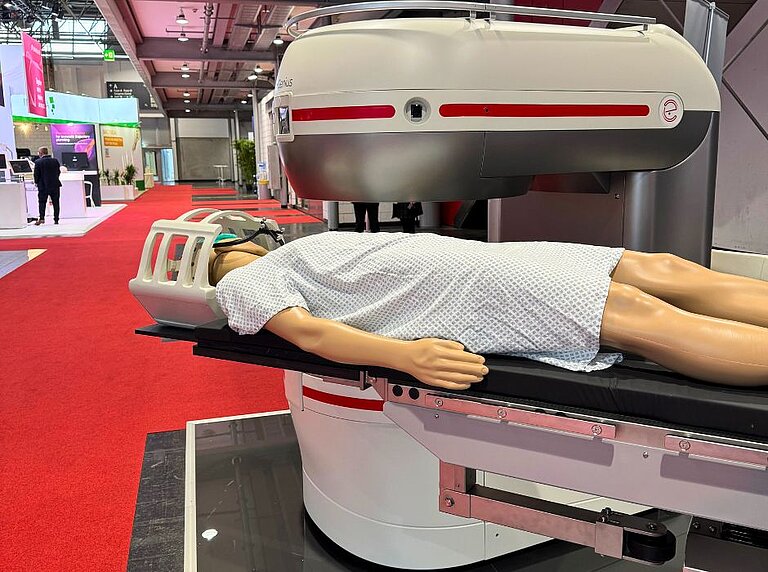
To overcome this challenge, Esaote developed I-Genius, an innovative intraoperative magnetic resonance imaging (iMRI) system designed to remain inside the operating room during brain surgery, particularly for the treatment of gliomas.
“The real challenge wasn’t the technology itself” says Marta Mensi, MRI Clinical Application Specialist at Esaote, “but designing a solution that makes iMRI truly usable and accessible in the operating room by eliminating patient transfer. In the development of I‑Genius, we didn’t start with the machine, we started with the clinical problem”. This reflects Esaote’s “Solutions For philosophy”: listening to healthcare professionals and translating their real needs into technology that supports the surgeon’s way of working and clinical reasoning.
I-Genius is the result of years of close collaboration among engineers, neurosurgeons, anesthesiologists, and clinical technicians. Together, they addressed imaging performance, surgical ergonomics, sterility requirements, patient positioning, and team communication. “Confidence comes from being supported by the right technology that fits the surgeon’s needs,” according to Mensi.
Workflow-focused technology that fits in surgeons’ hands
“What is truly innovative about I-Genius is its ability to provide intraoperative imaging at every stage of neurosurgery” - Dr. Roberto Rafael Herrera, Chief of Neurosurgery at Clínica Adventista Belgrano in Buenos Aires, explains – “Both surgical and MRI procedures take place on a single integrated bed system. There is no need to move the patient. This allows the surgeon to resect the lesion, immediately verify the result, reassess how to proceed with precision and safety, and then confidently continue the procedure. This process can be repeated as many times as the surgeon deems necessary during the operation, culminating in a final check”.
According to Herrera, this approach “provides the certainty of having achieved the maximum safe resection of the tumor while preserving the healthy brain and the patient’s neurological function”. I-Genius supports decision-making within the surgical flow – integrated, iterative, and guided by clinical judgment.
A plug-and-play iMRI for patient-centered precision

“For the neurosurgeon, it’s the assurance that what they see matches what the image reveals – even the details invisible to the eye”, Mensi explains. “For the patient, it means that every decision during surgery is guided by information, not assumption”, why precision and flexibility of MRI matter during the demanding, long surgeries requiring the highest concentration and teamwork.
Another priority, according to Mensi, was achieving precision and flexibility with one device, making the I-Genius adaptable across different clinical settings – from major university hospitals to specialized oncology units.
“Our goal was to make imaging solutions more accessible”, says Mensi, “Not only for large hospitals, but also for smaller clinics. We wanted to integrate low-field iMRI technology into every operating room.
What she values most about the system is its immediate usability. “It’s a game-changer for intraoperative procedures, enhancing workflow and efficiency. It’s fully ready for the operating theater, integrating with existing tools and practices from day one, so surgeons can use it immediately without additional setup”.
Making advanced neurosurgery more accessible
“We have built technology that enhances collaboration, patient outcomes, and improves access to the most advanced procedures,” concluded Mensi. “And that’s a good feeling of making progress that now can help more people”.
As she notes, “I-Genius augmenting surgeons’ capabilities.” This approach speaks to Esaote’s broader mission: to advance medical imaging while preserving the clinical perspective that defines patient care. For Esaote, the new technology marks the next step toward the future in which imaging, neuronavigation, and artificial intelligence work together to support surgical excellence. “While technologies advance, the values remain the same: first-class healthcare innovation comes from enhancing human capabilities with technology designed through empathy and an understanding of what truly matters in care”.
Genius in medicine lies in listening to healthcare professionals, in collaboration, and in the quiet power of doing things better for patients and clinicians alike.
Artur Olesch, Digital Health Journalist, Founder & Editor-in-Chief
aboutdigitalhealth.com
Read other articles

CARE
Behind the scenes of the medical infrastructure supporting a major sporting event: what it takes to ensure care at the Winter Olympics
The organisation of imaging and healthcare in a multi-venue event such…
CARE
How to design technology that saves lives: from the evolution of imaging to the I‑Genius case
In the 1990s, designing an imaging system mainly meant meeting a…

CARE
Caring for the carer: a still underestimated medical responsibility
Behind every person facing a serious illness, there are others who…
CARE
Prevention begins within the company: breast cancer screening in the workplace
October marks Breast Cancer Prevention Month - a time to spotlight a…

CARE
Technology and empathy: the new narrative of care with Esaote and PERSONE
We are living in an extraordinary age for medicine: we’ve never had…
